Liver disease treatment in South Mumbai
What is Chronic Liver Disease?
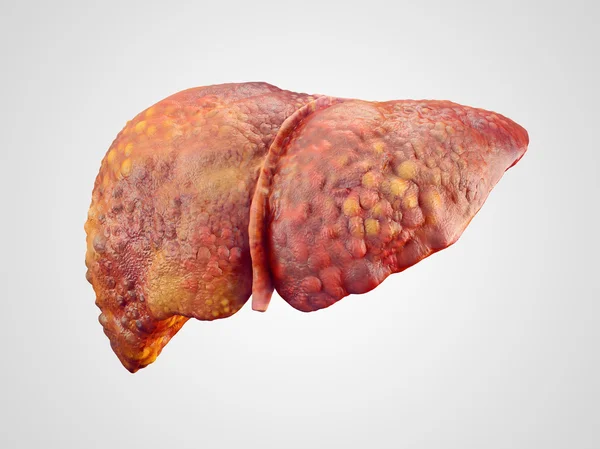
The liver is essential for digesting food and clearing your body of toxic substances. Cirrhosis is when scar tissue supplants healthy liver tissue. This prevents the liver from working normally. Cirrhosis is defined as long-term (chronic) liver disease. The loss to your liver builds up over time.
Our liver is the body’s largest internal organ. It is placed under our ribs on the right side of your belly. The liver performs many important things including:
- Waste removal from the body, such as toxins and medicines
- Making bile to help digest food
- Storing sugar that the body uses for energy
- Making new proteins.
When you are diagnosed with cirrhosis, scar tissue slowdowns the flow of blood through the liver. Over time, the liver can’t perform the way it should. In some cases, the liver is damaged so badly that it stops functioning. This causes liver failure.
Dr Chetan Kalal is a Liver disease treatment in South Mumbai, he is associated with Sir HN Reliance Foundation Hospital and Research Centre. Let’s see what causes cirrhosis.
What causes liver disease?
Parasites and viruses can infect the liver, causing inflammation that reduces liver function. The viruses that cause liver damage can be spread through blood or semen, contaminated food or water, or close contact with a person who is infected. The most common types of liver infection are hepatitis viruses, including:
-
- Hepatitis A
- Hepatitis B
- Hepatitis C
Diseases in which your immune system attacks certain parts of your body (autoimmune) can affect your liver. Examples of autoimmune liver diseases include:
- Autoimmune hepatitis
- Primary biliary cholangitis
- Primary sclerosing cholangitis
An abnormal gene inherited from one or both of your parents can cause various substances to build up in your liver, resulting in liver damage. Genetic liver diseases include:
-
- Hemochromatosis
- Wilson’s disease
- Alpha-1 antitrypsin deficiency
Examples include:
-
- Liver cancer
- Bile duct cancer
- Liver adenoma
Additional, common causes of liver disease include:
-
- Chronic alcohol abuse
- Fat accumulation in the liver (nonalcoholic fatty liver disease)
- Certain prescription or over-the-counter medications
- Certain herbal compounds
What are the symptoms of cirrhosis/ liver disease?
Liver disease doesn’t always cause noticeable signs and symptoms. If signs and symptoms of liver disease do occur, the may include:
Skin and eyes that appear yellowish (jaundice)
Swelling in the legs and ankles
Dark urine color
Chronic fatigue
Loss of appetite
Abdominal pain and swelling
Itchy skin
Pale stool color
Nausea or vomiting
Tendency to bruise easily
How is cirrhosis treated?
This information will help you care for yourself and know what to watch for when you are at home Be active
• Physical activity helps you keep and build muscle.
• Start walking at least 10 minutes a day, 3 to 4 days a week.
• Go for long walks and walk more often.
• Build up to walking every day and at least 150 minutes each week.
• Do resistance exercises and balance training 2 or 3 days each week.
Ask your healthcare provider for advice about being active
Eat healthy
Healthy eating is important to help you manage weight, prevent other health problems, and keep your body strong.
• Eat the right amount of protein and calories that you need.
• Eat every 3 to 4 hours during the day.
• Have a snack before bed and eat breakfast soon after you wake up.
• Don’t have more than 2000 mg of sodium each day.
Talk to your healthcare provider about how many calories and how much protein and other nutrients are right for you.
Take care of yourself
It’s important to know how to manage your condition and other health conditions caused by cirrhosis. These include fluid build-up, bleeding, and hepatic encephalopathy.
Tracking your health information will help your doctor manage your condition. Also, let your healthcare team know if you have:
• feelings of depression or anxiety
• muscle cramps
• pain
• weight loss
• itching
• trouble sleeping
Fluid build-up
Cirrhosis can cause fluid to build up in different areas of the body. This leads to swelling (also called edema)
• The fluid that builds up in the belly is called ascites.
• The fluid that builds up in the lungs is called pleural effusion.
If you’re being treated for a build-up of fluid, it’s important to weigh yourself each morning. Weight yourself before breakfast, before you drink anything or take medicine, and after you pee (urinate)
Keep track of your weight each day in a notebook or app on your phone. Let your healthcare provider know if you:
• lose 1 kg or more in a day, for 2 days in a row
• gain 1 kg or more in a day, for 2 days in a row
• see more swelling in your belly, legs, or feet
• have shortness of breath when you’re active or lying down
Some of the treatments for fluid build-ups include limiting salt, taking diuretic medicines (water pills), and draining fluid from your body (through a procedure called paracentesis or thoracentesis).
Your healthcare provider may have you do blood tests regularly, especially if you take diuretic medicines.
Check your blood pressure and pulse 2 to 3 times per week. Rest for at least five minutes before you check these measurements. Record your measurements in a notebook or app on your phone. Let your healthcare provider know if:
• Your pulse is less than 50 beats per minute.
• The first (or top) number of your blood pressure is lower than 90.
• You are dizzy, lightheaded, or falling.
Record the number of bowel movements you have each day in a notebook or app on your phone to show your healthcare provider. If you take lactihep/looz/duphalac adjust the amount you take so you have 2 to 3 medium to large, soft bowel movements a day. Don’t take more than you need because it may make you dehydrated. But if you don’t take enough, you may feel confused. Avoid medications that can make you sleepy. Let your healthcare provider know if you:
• Have trouble adjusting the dose of Lactulose to have 2 to 3 medium to large, soft bowel movements a day.
• Feel tired, sleep more, or your sleep patterns change so you’re up at night and sleep during the day.
• Have trouble concentrating or remembering things. § Have a change in your personality.
• Notice shaking of your body (called a tremor) or unsteady (feel like you may fall).
Ask your healthcare team for local resources to help you to do this.


